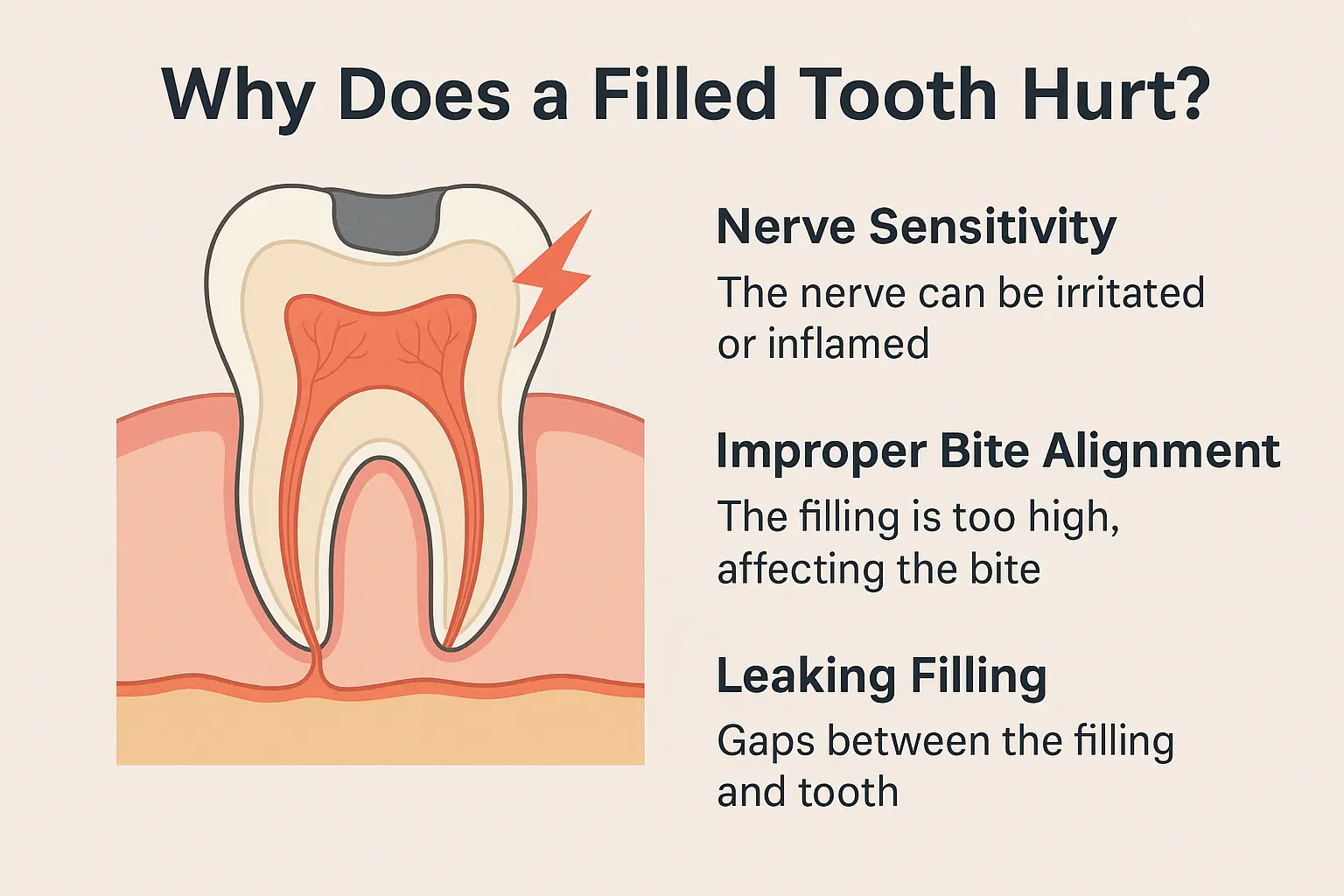
Why you can feel tooth pain when nothing is “wrong” with the tooth
Most people assume tooth pain always comes from a cavity or infection. Often that’s true. But sometimes the tooth is not the main source — the discomfort is referred from nearby structures (sinuses, jaw joint, ear), nerves, or muscle tension.
The key is to look for patterns (head position, chewing, cold sensitivity, stress, nighttime grinding, congestion) and then get a targeted exam to confirm the cause.
- Upper back teeth + congestion often points to sinus pressure.
- Jaw clicking/lock + temple ache often points to TMJ or clenching.
- Nighttime soreness + worn edges often points to grinding (bruxism).
- Sharp “electric” zaps may be nerve-related and needs medical evaluation.
Self-check table: what your symptoms may be pointing to
This is a practical guide (not a diagnosis). If you’re unsure, start with a dental exam to rule out hidden tooth issues.
| What you notice | Common hidden cause | Who to see first |
|---|---|---|
| Upper molars ache Worse when bending down; congestion/cold symptoms |
Sinus pressure / inflammation | Dentist + consider ENT if dental exam is clear |
| Jaw feels tired Clicking, tightness, headache, pain near ear |
TMJ disorder / clenching | Dentist (bite evaluation) + sometimes physiotherapy |
| Sore on waking Worn teeth, sensitive teeth, “dull” ache |
Bruxism (night grinding) | Dentist (night guard) |
| Sharp zaps Brief “electric” pain, triggers from touch/air |
Nerve-related pain | Dentist to rule out tooth; then GP/neurologist |
| Pain with chewing Feels “high” bite or localized tenderness |
Hidden crack / bite trauma / gum inflammation | Dentist |
9 hidden causes of tooth pain (even without a cavity)
1) Sinus problems (the “upper toothache” confusion)
When your sinuses are irritated, pressure can be felt around the roots of the upper molars — and it can mimic a toothache. A big clue is pain that changes with head position or comes with congestion.
2) TMJ disorders (jaw joint irritation)
The temporomandibular joint (TMJ) sits close to the ear and teeth. Clenching, stress, arthritis, or bite imbalance can irritate the joint and surrounding muscles, creating a dull, radiating “tooth” pain.
3) Bruxism (teeth grinding) — the silent trigger
Many people grind without noticing (especially during sleep). Over time it overloads teeth and muscles, causing morning soreness, sensitivity, and a deep ache.
4) Gum inflammation (pain that feels like it’s the tooth)
Inflamed gums can create tenderness that patients describe as tooth pain. If brushing causes bleeding or soreness between teeth, gum health may be a key part of the problem.
5) A tiny crack or bite trauma
Small cracks can be hard to spot without an exam. Pain may be sharp on biting or when releasing your bite, even if the tooth looks “fine.”
6) Ear-related pain (referred discomfort)
Ear irritation can sometimes be felt as tooth pain because nearby nerves overlap. If your dentist can’t find a dental cause, an ENT check may help.
7) Nerve-related pain and migraine-type patterns
Some nerve pains can show up as toothache-like sensations. If you get brief, intense “zaps” or tooth pain with no dental findings, get medical evaluation after a dental check.
8) Vitamin/mineral imbalance & hormonal sensitivity
In some cases, overall sensitivity can increase due to broader body changes. If your dental exam is normal and symptoms persist, your doctor may recommend broader evaluation.
9) Stress, anxiety, and poor sleep (pain amplification)
Stress can increase muscle tension, clenching, and your perception of pain — making minor sensitivity feel much worse.
What to do right now (safe steps)
- Track triggers: cold, chewing, bending down, nighttime, stress.
- Avoid overload: chew on the other side; avoid hard foods and gum.
- Use gentle hygiene: brush softly and floss carefully to remove trapped food.
- Cold pack (outside cheek): 10 minutes on / 10 off if swelling or throbbing.
- Pain relief: follow the medication label and your clinician’s advice (especially if pregnant or on blood thinners).
- Book an exam: if pain lasts more than 48 hours, keeps waking you up, or keeps returning.
When to see a dentist vs a doctor
See a dentist urgently if you have:
- Swelling in the face or gums
- Fever or feeling unwell
- Severe pain that’s worsening or waking you at night
- Pain when biting (possible crack/bite trauma)
- Bad taste, drainage, or persistent sensitivity
Consider a doctor/ENT evaluation (after dental check) if:
- Tooth pain clearly matches sinus/ear symptoms
- Dental exam is normal but pain persists
- You get nerve-like “electric” pain episodes
How we can help at Inter Dental Turkey (Side, Antalya)
Tooth pain without a cavity still deserves a proper dental exam — hidden cracks, gum inflammation, or bite overload can be easy to miss without targeted checks. Depending on your findings, we may recommend:
- Focused exam + diagnostics to identify the source
- Bite and TMJ evaluation if clenching/grinding is suspected
- Gum assessment if tenderness/bleeding is present
- Same-day pain-focused care when appropriate
Useful links: Emergency Dentistry · Gum Care · Contacts